Page 25 - 20211214_OHKF_Health_Finance_Research_Report_E (1)
P. 25
In recognition that conventional disease-focused care models are no longer sufficient to
address the emerging healthcare needs in the 21st century, the WHO has called for a
“fundamental paradigm shift in the way health services are funded, managed, and delivered”
to achieve further gains in health outcomes (WHO, 2015b). To reshape our health system to
tailor for the emerging needs amidst demographic and epidemiological transitions, our
research report Fit for Purpose: A Health System for the 21st Century
presented a visionary transformation of the system towards one that is primary care-led,
integrated, and person-centred. We put forward a conceptual integrated health services
model that emphasises building and connecting primary and community care hubs to
surrounding networks–in order to help the health system progress towards becoming fit-for-
purpose (Figure 1.3).
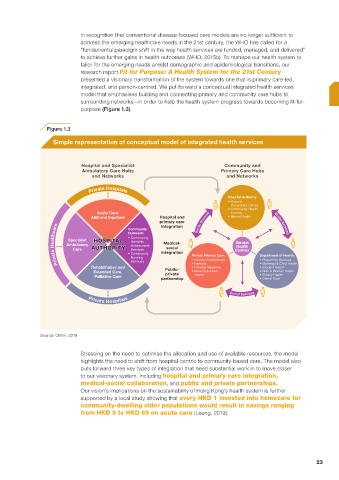
Figure 1.3
Simple representation of conceptual model of integrated health services
Hospital and Specialist Community and
Ambulatory Care Hubs Primary Care Hubs
and Networks and Networks
Private Hospitals
Hospital Authority:
• General
Out-patient Clinics
• Community Health
Acute Care: Centres
A&E and Inpatient Hospital and • Mental Health
primary care Social Services Social Services
Private Healthcare Ambulatory AUTHORITY Outreach: integration Private Primary Care: Centres Department of Health:
integration
Community
• Community
HOSPITAL
Specialist
Geriatric
District
Medical-
Assessment
Health
social
Care
Services
• Community
Services
• Dentists
• Maternal & Child Health
Rehabilitative and Nursing Public- • General Practitioners • Preventive Services
• Student Health
• Chinese Medicine
Extended Care, private • Nursing & Allied • Men & Women Health
Palliative Care Health • Elderly Health
partnership • Dental Care
Social Services
Private Hospitals
Source: OHKF, 2018
Stressing on the need to optimise the allocation and use of available resources, the model
highlights the need to shift from hospital-centric to community-based care. The model also
puts forward three key types of integration that need substantial work in to move closer
to our visionary system, including hospital and primary care integration,
medical-social collaboration, and public and private partnerships.
Our vision’s implications on the sustainability of Hong Kong’s health system is further
supported by a local study showing that every HKD 1 invested into homecare for
community-dwelling older populations would result in savings ranging
from HKD 9 to HKD 69 on acute care (Leung, 2019).
23